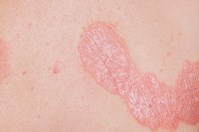
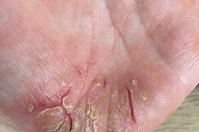
About Psoriasis
Psoriasis is more than just a skin condition, and it can affect people physically and psychologically. Although there is no cure for psoriasis, it is important to remember that it can be managed. With the right treatment and advice, many people live well with psoriasis.
We're committed to producing good quality information, and we've used our experience and best practice to pull together as much information as possible on treating and living with psoriasis and psoriatic arthritis. Please use the links below and in the menu to learn more!
It's important to remember that the information on this website is not a replacement for advice from a qualified health professional. Please also remember that posts on the forums and social media can come from a variety of sources and may not always be factually correct. You can learn more about our information by reading our Good Quality Information Policy.
Can psoriasis be treated?
How will psoriasis affect me?
September 2023 (Review Date: March 2026)