Psoriasis in Sensitive Areas
Psoriasis can affect sensitive areas of the body, such as the face, armpits, genitals and skin folds.
About psoriasis in sensitive areas
The skin is more sensitive in certain
areas of the body than others. Often, these are areas which are covered by
clothes or other skin, such as the armpits, genitals and skin folds. You might
hear these areas referred to as ‘flexural’ or ‘inverse’. The face is another
sensitive area.
How does psoriasis differ in a sensitive area?
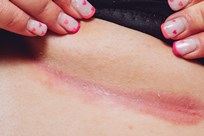
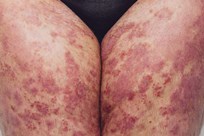
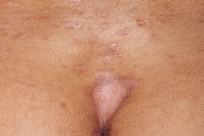
Psoriasis in flexural areas often
does not have the typical ‘plaques’ or scaliness seen in other areas and
usually appears as very bright red (or dark on darker skin tones) and shiny. It
is well demarcated (easy to tell where the psoriasis ends and normal skin
begins). Because psoriasis in these areas looks quite different to its typical
dry and scaly appearance, it can often be mistaken for a fungal infection or
other skin condition.
Psoriasis in sensitive areas may be very uncomfortable and
painful, and may make people feel embarrassed about or avoid intimate
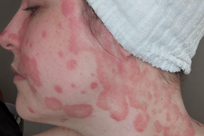
situations. Psoriasis in sensitive but non-flexural areas (such as the face)
may look similar to psoriasis on other parts of the body.
What triggers psoriasis in sensitive areas?
As with other types of psoriasis, it is not easy to pinpoint what triggers psoriasis in sensitive areas. Sometimes it happens spontaneously, or for no real reason at all. However, psoriasis in the armpits, other flexures and groin area may sometimes get worse as a result of external factors. These may include tight clothing rubbing the skin, deodorants or antiperspirants, sanitary towels or tampons, harsh toilet paper, thrush and sexual intercourse.
What should I do if I have psoriasis in a sensitive area?
It is always best to seek help from a GP or Dermatologist for psoriasis in sensitive areas. This is because psoriasis in these
areas can be painful or particularly uncomfortable, can affect a
person’s quality of life (such as their work, relationships and social
life), and may be more prone to infection. Treatments that may have been prescribed for psoriasis on another area of the body are not
always suitable for psoriasis in sensitive areas. Because of this, a
separate treatment plan may be needed for these areas. Suitable treatment may only be available on prescription, and so a visit to a GP or Dermatologist is essential.
Not all topical (applied to skin ) treatments for sensitive areas are suitable to use long-term, and so even if you are getting on well with your treatment, it is a good idea to review your treatment with your doctor on a regular basis.
How can psoriasis in a sensitive area be treated?
As with all types of psoriasis, it is important to regularly moisturise psoriasis in sensitive areas. This can help to make the skin more comfortable, and is also thought to help some topical treatments to be more effective.
Skin in the flexural areas is thinner, and is often covered by clothing such as in the armpit. Treatment is absorbed more
easily in these areas and therefore does not necessarily need to be as strong as is needed in other areas to be effective. Mild to moderate potency (strength) steroid creams are often used for sensitive areas. However, care should be taken with their use in flexures as the warm environment can increase the strength and may lead to side effects such as skin thinning. Topical steroids should not be used for long periods of time or without regular reviews by your doctor. Steroid treatment should never
be stopped abruptly as this may trigger a rebound of your
psoriasis, and so should be ‘weaned’ off, by gradually reducing the number of doses.
Topical Vitamin
D creams and ointments can be
used alone or in combination with a steroid. Used alone, they have few potential side effects and so can be used for longer Some vitamin D
topicals are suitable for use in sensitive areas, but some are not – so
it is important to clarify this with a GP or Pharmacist.
In recent years, a group of treatments known as calcineurin inhibitors have been launched for another skin condition, called atopic dermatitis. These reduce inflammation, and may sometimes be prescribed ‘off licence’ for other inflammatory skin
conditions, such as psoriasis. These can be used in sensitive areas for
longer than topical steroids, and can therefore make a good
alternative; although they can increase skin sensitivity to UV light, meaning exposure to the sun, sunbeds, or ultraviolet light treatment
must be limited.
Anti-fungal and anti-bacterial treatments may also be prescribed, as infections are more common in sensitive areas. If present, these will need to
be treated alongside the psoriasis.